Peripheral Artery Disease (PAD)
Do your legs cramp when you walk? Have they become weak, or even numb? Do your feet feel cold or change color? You may have PAD, where a blood vessel in your leg has become “clogged” with cholesterol plaque. Sometimes folks feel they are just “getting older” and ignore the symptoms of pain, fatigue or skin discoloration, when in fact they may be developing a dangerous blockage in their arteries.
What is peripheral artery disease or PAD?
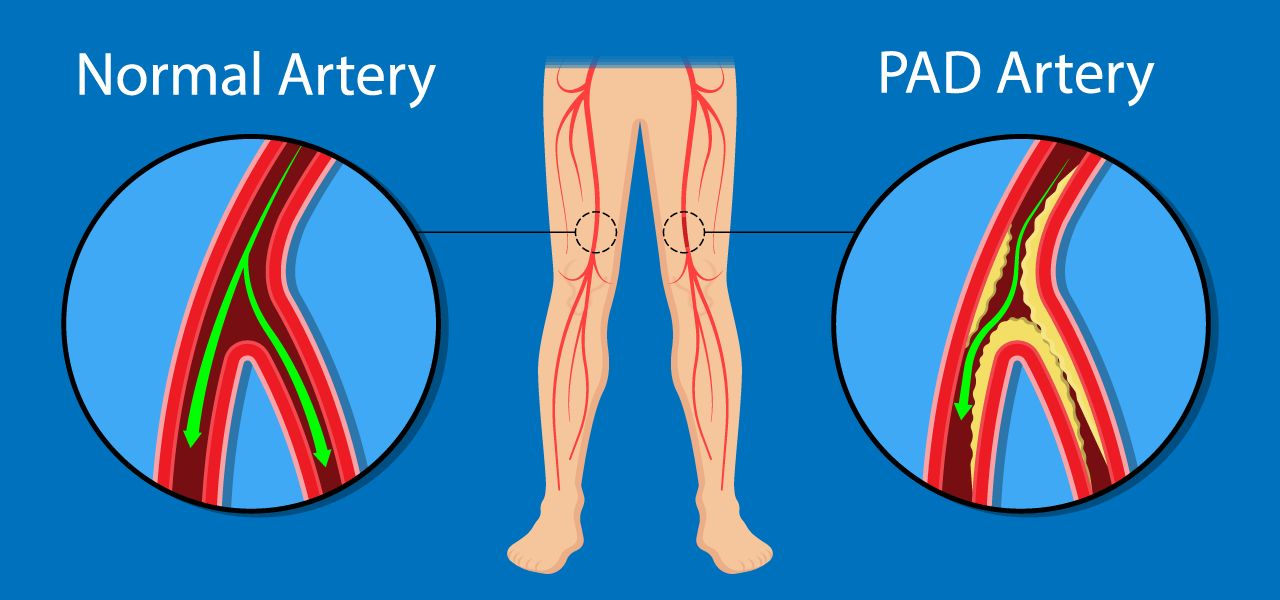
PAD results from cholesterol buildup, which restricts the amount of blood reaching your legs, feet and toes. When oxygen and nutrients can’t reach your muscles, it may be difficult to walk and your legs can feel tired, crampy or numb. You may even want to sit down after strolling only a short distance. Pain with walking, relieved by rest, is called claudication, a classic symptom of PAD. You may find it more difficult to exercise or climb stairs because of the pain. However, up to 40 percent of those with PAD have no leg pain whatsoever. Instead, they may have weak or numb legs, cold feet, may lose hair on the legs or develop yellow thickened toenails. Over time, the skin can take on a pale, red or shiny appearance. This occurs as the blood flow to the legs is pinched off, and again almost half of PAD patients experience changes in the skin or nails, without experiencing leg pain.
What happens if PAD is not treated?
PAD is a serious condition, and when critical blockages develop, the skin can break down, gangrene can set in and the toe or foot may need to be amputated. In fact, arterial disease is the leading cause of leg amputations in the U.S. Even worse, almost half of those with a leg amputation die within a year of the amputation. Fortunately, with timely treatment, most amputations can be avoided. Just as important, controlling PAD risk factors can lessen the risks of heart attack and stroke. It is important to identify PAD early, to help control risk factors and re-establish good blood flow before permanent damage is done.
Am I at risk for peripheral artery disease (PAD)?
If you smoke, are diabetic, have high blood pressure or kidney disease, you are at higher risk for developing PAD. Diabetes is especially troublesome, as 1 in 3 diabetics over the age 50 have PAD. Smoking further increases the risk of blocked vessels by 400 percent. Unfortunately, those who develop PAD have 5 times greater risk of stroke and heart attack. This is why it is so important to control PAD risk factors. Healthy lifestyle changes not only improve the circulation in the legs, but also can help prevent clots in your heart and brain as well.
What can I do to prevent PAD?
Here is where YOU can make a BIG difference. Start small. Even only 5-10 pounds of weight loss can improve blood pressure as much as a prescription medicine. And, weight loss can increase energy levels, physical mobility and self-confidence. So, take a walk, set a goal for a 5 pound weight loss and add a healthy snack to your routine. If you smoke, try one of these proven treatments that can help you quit. Check out CDC.gov/quit, get free confidential coaching at 1-800-Quit-Now or simply text QUIT to 47848 to receive daily text messages to support you in your quitting journey. If just one patient who reads this section stops smoking, it would have made writing this section well worth it! Let us know what worked for you and we will be happy to share with others.
How can I tell if I have peripheral artery disease (PAD)?
We have painless, noninvasive tests to identify blockages in the arteries. The simplest is an ABI, or “ankle-brachial index” which compares blood pressures in the arms and legs. Because of gravity, the pressure in the ankles should always be higher than that of the arms. If the blood pressure in the legs drops below that of the arms, this indicates an obstructed leg artery. Another useful exam, an “arterial duplex,” utilizes ultrasound to map out areas of narrowing in the arteries. Both exams are performed in our office, and if a significant blockage is detected, we arrange for appropriate treatment with our arterial vascular colleagues.
Do I need to have surgery for PAD?
If plaque is found in the arteries, today there are less invasive ways of opening these “plugged” vessels. In the past, the only option was major bypass surgery. This operation carried significant surgical risks and required a prolonged hospital stay and recovery. Today, outpatient angioplasty and stenting are available. These minimally invasive procedures use small fiber optic instruments to clear the blockage. These techniques begin with a small needle poke rather than a large incision. We refer to specialized outpatient vascular centers, which allow patients to return home the very same day.
Facts about PAD:
- PAD, cholesterol blockages in the arteries of the leg, affects about 10 million people in the U.S.
- Diabetes, smoking, high blood pressure and kidney disease all raise the risk of PAD.
- Leg pain with walking is classic, but weakness, numbness or cold feet also point to PAD. Ignoring these symptoms can allow more significant blockages to develop.
- Unattended, severe blockages can cause ulcers and gangrene. PAD is the leading cause of amputations in the U.S.
- Most amputations can be prevented with early intervention and healthy lifestyle changes. Walking, quitting smoking and eating a healthy diet really help!
- Advanced Vein Center performs noninvasive screening tests for PAD and refers to centers that perform minimally invasive treatment.
Ready to take the first step toward better circulation? Schedule your appointment today — 480-844-VEIN (8346).